A community-based joint care initiative integrating nutrition and welfare services has significantly improved health satisfaction among elderly participants with chronic conditions. Recent analysis reveals a 16% rise in overall health indicators and a 33% surge in self-efficacy among full-time program attendees.
Program Details and Structure
The “Na Dolbom (Body-Mind-Spirit)” program targets seniors aged 65 and older attending local welfare centers. Delivered over 12 weeks, it combines physical rehabilitation, mental counseling, nutritional guidance, and spiritual activities to foster holistic well-being. Key components include body-focused physical therapy and rehab, mind-oriented stress management and emotional support, and spirit-driven sessions to rediscover life’s purpose.
Experts from Hallym University Dongtan Sacred Heart Hospital, including team leader Kim Joo-nyoung, nutrition society welfare director; Hwaseong-si Dongtan Elderly Welfare Center director Kim Ho-sun; Hallym University social welfare professor Kim Ye-jin; and researcher Park Sa-jeong collaborated on this effort. They surveyed 45 chronic disease patients using the center, assessing changes in health satisfaction, self-efficacy, and concentration through standardized 100-point scales.
Key Results from Participant Assessments
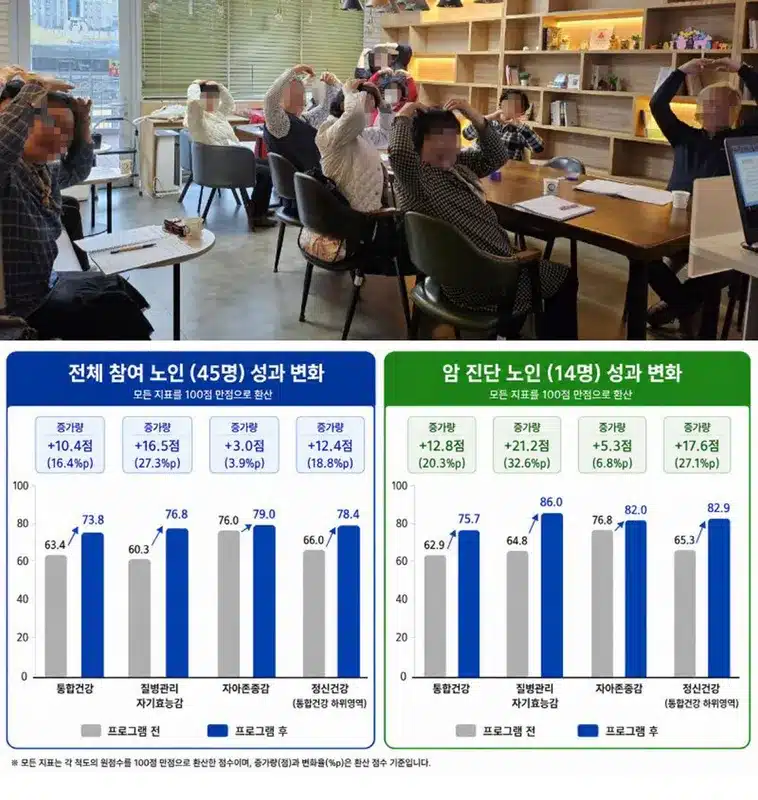
Overall health satisfaction climbed from an average of 63.4 to 73.8 points, a 10.4-point increase (16.4%). Self-efficacy feelings rose sharply from 60.3 to 76.8 points (16.5-point gain, 27.3%), while concentration improved modestly from 76.0 to 79.0 points (3.0-point rise, 3.9%). These shifts indicate comprehensive health gains across physical, mental, and social domains.
Breakdown by Category
- Mental health scores jumped from 66.0 to 78.4 points (12.4-point increase, 18.8%), highlighting the program’s impact on psychological well-being.
- Among 14 participants receiving meals, gains were even stronger: health satisfaction rose 12.8 points (20.3%) to 75.7; self-efficacy increased 5.3 points (6.8%) to 82.0; and self-efficacy feelings surged 21.2 points (32.6%) to 86.0.
Researchers note that integrating hospital nutrition education with welfare services addresses medical, nutritional, and emotional needs, enabling deeper life engagement for seniors.
Participant and Expert Insights
Participant A, a meal recipient, shared: “After starting meals here, I no longer feel tired or annoyed with people. Regaining my body’s strength gives me confidence that ‘I can do it too,’ reigniting my courage. Even touching changes feels straightforward now, and a fresh sense of hope has emerged.”
Kim Joo-nyoung, team leader at Hallym University Dongtan Sacred Heart Hospital’s nutrition society, stated: “Seniors often face psychological burdens like anxiety and unease alongside physical decline, making full recovery challenging. By addressing body, mind, and spirit through this program, participants rediscover joy in daily life, motivating us to expand community-linked initiatives.”
Kim Ho-sun, director of Hwaseong-si Dongtan Elderly Welfare Center, added: “Joint care programs like this provide essential nutrition, medical, and welfare services in one stop, proving invaluable regardless of age. Collaborating closely with hospitals allows us to reach more seniors with tailored support.”
This study marks the largest joint nutrition-welfare effort published in a leading gerontology journal, demonstrating potential for broader adoption in elderly care.